Brief H&P
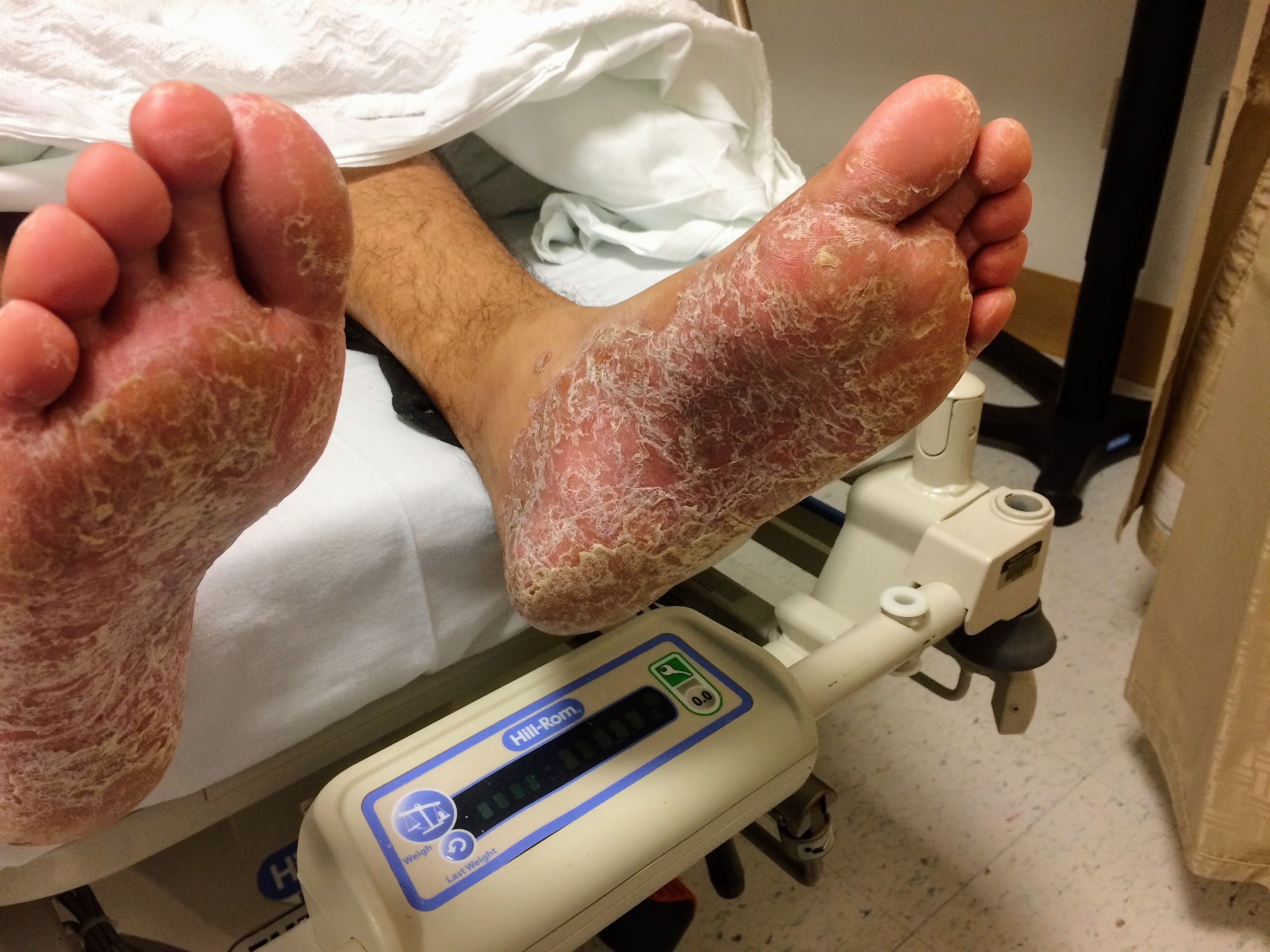
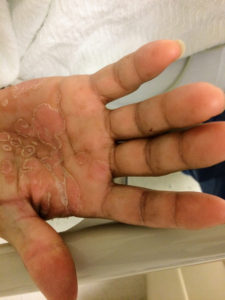
A young male with a history of HIV (untreated for the last year, with unknown CD4 count), and syphilis (reportedly treated with an intramuscular injection 1 year ago), presents with 4 months of a painful rash on the palms and soles and diplopia. Examination revealed the rash pictured below, ocular examination with minimal papilledema and anterior chamber inflammation.
Labs were unremarkable. CSF sampling was notable for 34 WBC’s with lymphocyte predominance (92%), and elevated protein (56mg/dL). The patient was admitted for syphilis with presumed neurosyphilis. Serum RPR titer was elevated at 1:64, FTA-ABS and CSF VDRL were reactive. The patient was treated with intravenous penicillin and anti-retroviral therapy was reinitiated.
Epidemiology1
- Transmission
- Sexual contact (estimated transmission probability 60% per partner)
- Trans-placental
- Race/Sex
- African-American, Hispanic
- Male > Female
- Male (primary syphilis), female (secondary syphilis) – lesion visibility
- Urban > rural
Natural History1
| Stage | Signs/Symptoms | Incubation Period |
|---|---|---|
| Primary | Chancre, reginal lymphadenopathy | 3 weeks |
| Secondary | Rash, fever, malaise, generalized lymphadenopathy, mucous membrane lesions, condyloma lata, headache, meningitis | 2-12 weeks |
| Latent | Asymptomatic | Early (<1 year) Late (>1 year) |
| Tertiary | Cardiovascular: Aortic aneurysm, aortic insufficiency, coronary artery ostial stenosis | <2 years |
| CNS: | ||
| Acute syphilitic meningitis: headache, confusion, meningeal irritation | <2 years | |
| Meningovascular: cranial nerve palsy | 5-7 years | |
| General paresis: headache, vertigo, personality changes, vascular event | 5-7 years | |
| Tabes dorsalis: dementia, ataxia, Argyl-Robertson, [arrow-down] proprioception | 10-20 years | |
| Gumma: Local tissue destruction | 1-46 years |
Diagnosis1
- Serologic
- Non-treponemal (screening)
- RPR, VDRL
- Limitations: sensitivity, false positive (age, pregnancy, drugs, malignancy, autoimmune, viral infections)
- Treponemal (confirmatory)
- FTA-ABS
- Neurosyphilis
- Indications for CSF sampling: neurologic/ophthalmologic symptoms, tertiary syphilis (aortitis, gumma, iritis), HIV coinfection with elevated RPR titer (> 1:32)
- CSF: leukocytosis (predominantly lymphocytes), protein
- CSF VDRL reactive
- Negative CSF FTA-ABS may rule out neurosyphilis
- Non-treponemal (screening)
Syphilis in HIV-infected Individuals2
- Primary: larger and more lesion, multiple ulcers
- Secondary: genital ulcers more common, higher RPR/VDRL titers
- Tertiary: possibly more rapid progression to neurosyphilis
References
- Singh AE, Romanowski B. Syphilis: review with emphasis on clinical, epidemiologic, and some biologic features. Clin Microbiol Rev. 1999;12(2):187-209.
- French P. Syphilis. BMJ. 2007;334(7585):143-147. doi:10.1136/bmj.39085.518148.BE.